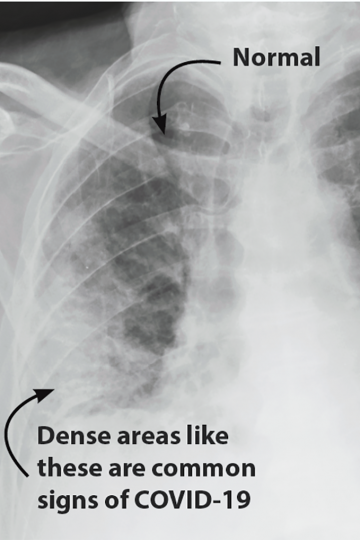
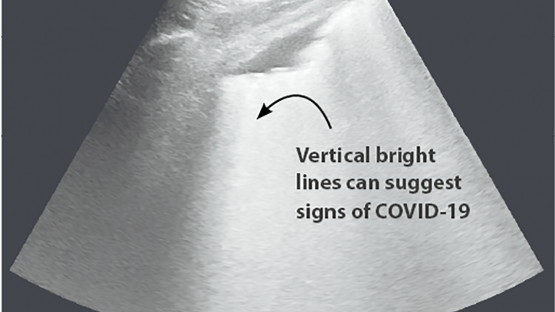
Getting images of what’s happening inside of people’s bodies is helping health professionals to evaluate and better understand the COVID-19 disease, which is caused by a newly discovered coronavirus.
“Diagnostic imaging is a window into the body,” said Olivier Pellet, a radiologist at the IAEA. “It has allowed us to uncover complications, such as lesions, pneumonia or blood clots in the lungs. Every day we learn about the virus and its impact on the human body, while discovering new COVID-19-related signs and symptoms we have not seen before, even when a person may otherwise appear asymptomatic.”